Samaritan is a proud provider of Dementia Care and uniquely distinguished as a GUIDE provider by the Centers for Medicare and Medicaid (CMS). Click to learn more.
(856) 596-1600 available 24/7 Refer Now

 Samaritan is proud to care for Muslim patients and their families. Being familiar with or asking about their Islamic beliefs and rituals can help you provide them better care and quality of life.
Samaritan is proud to care for Muslim patients and their families. Being familiar with or asking about their Islamic beliefs and rituals can help you provide them better care and quality of life.
Here are a few beliefs and rituals to use as your guide for healthcare and end-of-life care in the Islamic religion. These were complied with input from Katherine “Trinka” Klima, DNP, CNM, RN, Cherry Hill Free Clinic board member and a member of Samaritan’s Board Inclusion & Diversity Committee.
It’s very important to know that you should not feel obligated to become an expert on an unfamiliar faith tradition. A better goal is to be open, present, and curious.
Dr. Klima says, “In general, Muslims do not expect non-Muslims to cater to our beliefs or know a lot about Islam. We appreciate questions and respect people who are honest about what they don’t know.”
ILLNESS
For Muslims, health is a state of physical, psychological, spiritual, and social well-being. Muslims believe illness is a test from God and an opportunity to purify one’s sins. Muslim patients are encouraged to receive illness with patience and faith and to increase good deeds such as charity and prayer. At the same time, illness, pain and suffering should be relieved when possible. Even Muslim patients who are not actively practicing their faith may call for spiritual or religious intervention when they are facing significant challenges.
Dr. Klima adds, “The prophet Muhammad, peace be upon him, said ‘No blessing other than faith is better than well-being.’ Well-being encompasses physical and mental health, and yet it is much more than that. For who has not known a person with a terminal or disabling illness who seems to enjoy a high level of wellness and brings light to any gathering? And who has not known a person who seems to have excellent health and yet does nothing but complain? The Muslim is encouraged to be grateful to Allah for every blessing and challenge that she or he encounters, even while seeking a cure for illness, in the knowledge that Allah is most compassionate and most just.”
MEDICATION
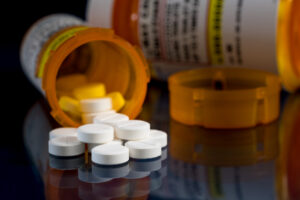 Medications that contain gelatin or are pork-based are forbidden. However, necessity to preserve life overcomes prohibition when there is no alternative. When considering medications, shared decision-making between the physician/nurse and the patient is the safest and most effective way to determine what to take and when. Patients want to talk to their healthcare providers and get trustworthy information.
Medications that contain gelatin or are pork-based are forbidden. However, necessity to preserve life overcomes prohibition when there is no alternative. When considering medications, shared decision-making between the physician/nurse and the patient is the safest and most effective way to determine what to take and when. Patients want to talk to their healthcare providers and get trustworthy information.
Deborah Parisi, Samaritan nurse and Staff Diversity Committee member adds, “Trust is important. So are open and respectful conversations. When reviewing pain medications with my Muslim patient and his family, I put the pharmacy on speaker phone so we could look closer at the ingredients in the medication.”
HOSPICE CARE
When it comes to end-of-life preferences and care in the Islamic faith, some patients prefer to die at home with the support of their families and very little or no help from healthcare providers. However, those who do choose hospice care do not expect you to tell them or remind them of their terminal illness. They believe God has predestined death and that hospice care may help the family fulfill a cultural and religious obligation if the focus is on comfort.
Dr. Klima explains, “Muslims are encouraged to treat treatable conditions, but to also be realistic when treatment is not an option, accepting this as God’s decree with patience and faith. Since we do not consider death to be the end of our lives, but only the end of this stage of our lives, part of our hopefulness is that we can continue to accumulate good deeds until our death, and that these will be rewarded in the next life.”
OTHER END-OF-LIFE CONSIDERATIONS
“Dying Muslims may like to listen to the Qur’an and family members may recite Quran or various prayers for the person, but these are not rituals. Muslims prefer to die facing Mecca, and it is a nice gesture to offer to turn the bed so that the person is facing approximately east/northeast from our area,” says Dr. Klima.
After death, the patient’s eyes should be closed, and their body should be covered. Friends or family should recite a final prayer for the deceased.
PRIVACY & DRESS

Most Muslims feel strongly about privacy and modesty. A few simple things can be done to make a Muslim patient’s end-of-life care or overall healthcare feel more comfortable. These include:
Many Muslim patients receiving or in end-of-life care will not want to shake hands with staff who are not the same gender, and some will avoid eye contact. This is intended as a sign of respect, not dismissiveness.
FASTING
Ramadan is the most sacred month of the year for Muslims. During this time, they abstain from all food and liquids from dawn to sunset throughout the month. People with illnesses that would be made worse by fasting, or those who must take medications on a schedule that prevents fasting, may make up the days later if their situation is temporary or feed a poor person for each missed day.
Healthcare providers should discuss fasting with their Muslim patients prior to Ramadan to help them to achieve their goals. Again, shared decision making between the healthcare provider and patient is the most effective way to help patients decide if they can fast safely.
PRAYER
Muslims pray five times a day facing Mecca (dawn, midday, mid-afternoon, sunset, night). They perform ritual ablution (washing parts of the body) before the prayer. Once prayer begins, be respectful of giving a patient privacy and a place to pray. Avoid interruption and do not walk in front of a person in prayer. Go next to or behind them, if necessary. Prayer typically only takes a few minutes.
In inpatient settings, staff can help by providing extra towels and a prayer rug or bed blanket for a patient and their family to pray on. Patients who cannot stand and bow for prayer may sit or lie in bed. But it is important that the bedding is clean of blood, urine, and stool or else the prayer would be considered invalid. Bedridden patients may need assistance to purify prior to prayer.
ASK QUESTIONS, BE OPEN
Colleen Fritsch, MSW, LCSW, Samaritan social worker and Staff Diversity Committee member, adds, “It also important to note that not every Muslim family believes in, or observes, all of the same things. I recommend asking the patient and family if there are any specific practices that they would like you to be aware of. Asking not only demonstrates a willingness to join with them, it also honors our commitment to diversity.”
It’s very important to know that you should not feel obligated to become an expert on an unfamiliar faith tradition. A better goal is to be open, present, and curious.
If you have any questions about providing healthcare to patients practicing Islam, or caring for Muslim patients and their families at the end of life, please contact Samaritan at (856) 596-1600.